Learning From What Goes Wrong
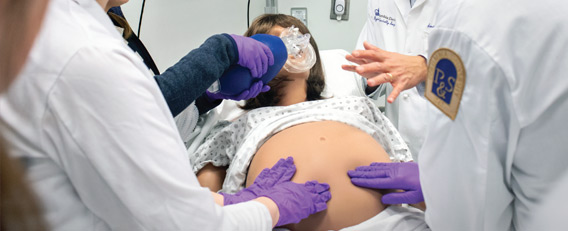
On any given day, one might find Victoria undergoing yet another complicated childbirth at the Vagelos Education Center (VEC). Perhaps this time it’s shoulder dystocia, a rare obstetric emergency in which the infant’s shoulder gets stuck on the mother’s pelvic bone, causing the baby to retract back into the canal like a turtle’s head retreating into its shell.
A small group of third-year medical students hover over Victoria wearing smocks and surgical masks. Some check vitals, while others take turns trying to maneuver the baby out of its perilous position. They are working in a mock operating room identical to the suites at NewYork-Presbyterian just down the road: The equipment is the same, including the crash carts in which each tool is arranged as it would be at the hospital.
The OR suite, like all rooms in the VEC simulation center, is outfitted with several cameras and microphones that feed into an adjacent control room where a simulation technician sits with a laptop. Using software on the laptop, the tech can put Victoria S2200—the lifelike, wireless “high-fidelity” manikin—through dozens of birthing scenarios. One click of the mouse causes her breathing to slow and her pupils to contract. Another click and her pulse jumps. Once the infant—an eight-pound manikin named Super Tory—is successfully delivered, it might cry or coo. Or it could have jaundice.

“We teach scenarios when everything goes right,” says David Deitsch, director of operations at the Mary and Michael Jaharis Simulation Center in the VEC, “but it’s more important to teach when everything goes wrong. Anything a physician might encounter while delivering a baby we try to replicate here.”
Simulated scenarios like this have become an integral part of medical education. Long used for training in other high-risk endeavors, such as aviation or combat, simulation has only recently been applied to a doctor’s education in a meaningful way. Whether it’s sophisticated manikins like Victoria or virtual reality-based software that guides a surgeon through a complex procedure, simulation-based medical education and its associated technology have now come of age, forming an increasingly significant part of medical school curricula and residency programs.
“Simulation is the future of what we need to be doing in health care,” says Arnold Advincula, MD, the Levine Family Professor of Women’s Health in Obstetrics & Gynecology and medical director of the Mary and Michael Jaharis Simulation Center. “This is not a ‘nice to have’ item. It’s a must-have, whether it’s about formative training or looking ahead to when students and new graduates are at the hospital seeing patients.”
 Arnold Advincula and David Deitsch
Arnold Advincula and David Deitsch
A Home for Simulation
Though simulation has been shown to help students retain information and hone skills while improving patient outcomes by decreasing costly medical errors, VP&S did not have a dedicated space to run simulated scenarios until the VEC opened in August 2016. Before then, medical students traveled to offsite facilities or did “in situ” training in makeshift spaces and unoccupied patient rooms at NYP.
The Vagelos Education Center—14 stories of angular glass and steel—has been covered extensively by architectural publications for its aesthetic qualities and energy-thrifty innovations. But it’s more than a lovely building with classrooms, study lounges, administrative suites, and auditorium laced together by an open staircase.
The simulation center, which occupies five floors, is at the heart of the building. The state-of-the-art facility has consolidated many of the activities that had been scattered across the medical center campus and introduced new ones. It hosts fundamentals classes, surgical skills labs, the Ready for Residency course, an anatomy quad, Objective Structured Clinical Examinations (OSCE), and more. Across the four years of medical school, each student will spend countless hours in the center.
It has become valuable for established health care professionals, too. Unlike most simulation centers, which are owned by either a medical school or a teaching hospital, this one is jointly operated by VP&S and NYP. When the hospital gets new technology, the simulation center gets it, too. In return, the center offers professional development to NYP departments and staff, from surgeons to nurses to residents, giving them the opportunity to experiment with new devices or procedures in a controlled, no-risk environment.

Dr. Advincula, a gynecologist and an expert in minimally invasive surgery, watched the VEC get built from the ground up. As medical director of the simulation center, he, along with a team of associate medical directors, were in charge of everything from laying out spaces to hiring staff to choosing which technology it would feature.
VEC architects had to be efficient in planning space for the building’s 125-by-100-foot lot. Likewise within the simulation center each room was designed with flexibility in mind, to support as many disparate activities as possible. In the basement, for instance, a large multipurpose space can be used as a single trauma bay to simulate mass casualty events or partitioned into two patient rooms for mock examinations. The debrief rooms, each with monitors and web cameras for video conferencing, and the two mock operating rooms, which host simulations and surgical skills labs, are similarly adaptable.
“You watch somebody do it, then you do it yourself, and all of a sudden you’re the expert? That’s really an antiquated way of learning.”
To run this space, Dave Deitsch brings 42 years of experience to his role as director of operations. Sean Feuer, the AV manager, was hired from Columbia’s School of International and Public Affairs, where he oversaw audio-visual systems. Around them a crew of simulation technicians, lab managers, and coordinators from this emerging field was carefully assembled.
They work with faculty to find the best ways to leverage new educational technology. “This process is still really embryonic,” says Dr. Advincula. “There’s a great number of faculty who are just now getting exposure to simulation. We know that it’s critically important to have them understand how to build a curriculum, how to design these scenarios, and also learn about the technology, so we’ve been working a lot on professional development. As we get more experience, it’s going to make things even better. It’s an exciting space to be in.”
Now in its third year, the simulation center is hitting its stride. Simulation is included throughout the medical school curriculum, from the first semester, when students are exposed to standardized patients—actors portraying patients—through the Major Clinical Year, when many of the hi-fi simulators are introduced, and beyond.

As faculty and staff experience expands, the scenarios grow ever more refined. The roster of hi-fi manikins—20 in all, capable of blinking, crying, breathing, and showing responses to drugs, CPR, or blunt force trauma—are put to use in more focused and imaginative ways, in situations that seek to capture the intensity of medical situations. This enables students to learn not only how to apply their budding clinical skills under pressure, but also how to work in a team, how to lead, how to communicate effectively when it matters most.
Scenarios are recorded from multiple angles, to be analyzed by the students in a faculty-led debriefing session afterward. This debriefing is essential to the process, allowing students to assess their performance and put it into context. In this way, simulation is much more than flashy technology; it is a didactic technique that relies on psychology as much as clinical skill.
This style of teaching has the potential to upend the apprenticeship model of “see one, do one, teach one,” which has dominated medicine for centuries.
“You watch somebody do it, then you do it yourself, and all of a sudden you’re the expert?” says Dr. Advincula. “That’s really an antiquated way of learning, because there are complications that only happen once in a while. The likelihood of a medical student spending five weeks on a rotation without ever seeing a shoulder dystocia, for example, is a real possibility.”
Therein lies the great benefit of simulation: It is as useful for teaching the common as it is the extraordinarily rare. Now, long before ever touching a patient, students have practiced common clinical techniques endlessly and have been exposed to a multitude of rare conditions a physician might see only once in a lifetime.
New School and Old School
Changes in technology have upped the need for simulation. Practice can give students confidence and dexterity in suturing a wound, but the finesse needed to operate a robot like the da Vinci Xi, which uses a few tiny incisions, a 3D vision system, and small-wristed instruments to perform surgery, is on another plane. Dr. Advincula and other surgeons rely heavily on the da Vinci robot. But with the presence of high-fidelity robotic simulators at the VEC that incorporate augmented reality, VP&S students now have an opportunity to practice on the robot. They can experiment with the robot in a low-stakes, structured environment and soon with the pending delivery of the actual da Vinci Xi robot, VP&S students will be able to experience full immersion into the world of robotic surgery.

Training students in skills, as much as teaching concepts, is critical to the center’s mission. During students’ final year and a half at VP&S, as they prepare for residency, they return to the center for specialty skills labs. Much of this training utilizes several dozen of the center’s low-fidelity task trainers, anatomical models students use to practice specific skills, like inserting an IV or central line.
“There’s a huge difference now in the quality of the first-year residents,” says Mr. Deitsch. “Simulation plays a big part in that. Students are able to get hands-on training they weren’t able to get before.”
For more complex procedures, like endoscopic or cardiac surgery, the center has several video-based simulators that pair graphics with haptic sensations, to mimic the feeling of guiding a hose down, say, a digestive tract. Like an app on a phone, these programs can be updated with new modules covering different procedures without changing the hardware.
These simulators hint at virtual reality- and augmented reality-based technologies, which are still in their infancy. But experts believe VR and AR will play a major role in how medicine is taught and practiced in the future. Mixed-reality headsets have the potential to transform how anatomy is taught. The simulation center hosts cutting-edge device manufacturers from around the world to run trials of new gadgets, becoming something of a beta test site. The novel technologies might not be ready for primetime use, but they provide a glimpse of the future.
Regardless of new tech’s potential, it is not likely to replace the experience of working with human cadavers in the simulation center’s state-of-the-art anatomy laboratory. Students use the laboratory to learn basic anatomy, and NYP staff, residents, and fellows use it for advanced surgical skills training.

Learning From Human “Patients”
In addition to learning to place a central line or replace a hip, students also must learn how to treat humans of all stripes: imperfect, confused, grief-stricken humans, drug-addicted humans, frustrated humans suffering from an illness they don’t quite know how to describe.
“You can only learn so much from a simulator, or a piece of plastic, or a cadaver. That feedback you get from a live human is crucial to the development of a medical student.”
“How do you tell a patient they have cancer and will only have three months to live?” says Mr. Deitsch. “You can only learn so much from a simulator, or a piece of plastic, or a cadaver. That feedback you get from a live human is crucial to the development of a medical student.”
While standardized patients have been part of medical education for years, VP&S only recently started its own formal program, coordinated by an actor who had been a standardized patient for years.
Students are matched with standardized patients, actors drawn from New York’s deep well of talent, who portray a multitude of ailments and conditions during the students’ OSCEs. These exams take place in 14 specially designed patient rooms throughout the center, each featuring glass so professors and other students can watch the interaction.
Until the opening of the simulation center in the Vagelos Education Center, VP&S students were sent offsite to prepare for the Step 2 Clinical Skills of the U.S. Medical Licensing Examination that uses standardized patients. Third-year medical students would participate in a day-long clinical assessment program at the Morchand Center of Icahn School of Medicine at Mount Sinai and later at Weill Cornell Medical College.
Each third-year student performed a focused medical evaluation on seven patients during the intense visit at the centers. Students and VP&S faculty members later reviewed the video recording of the performances. This arrangement continued until 2016, when the VEC opened.
The exams seek to mimic a bustling hospital ward, with the student moving frantically from station to station. The actors, who are also trained to evaluate the students, come in all ages and ethnicities and depict all kinds of conditions. Like the manikin-based simulations, these encounters escalate in difficulty, from basic physical exams with an agreeable patient to delivering bad news to a bereaved parent to treating someone who speaks a foreign language. Like OR scenarios, OSCEs are filmed and evaluated in debriefing sessions afterward. And, like all activities in the simulation center, the goal is to help students learn how to move from simulation to real-world care of patients with both competence and confidence.
——————
The simulation center offers everyone an opportunity to learn and refine their skills. Students interact with actors portraying patients to learn doctor-patient communication. They see Victoria or her robotic infant through a difficult childbirth to learn how to handle emergency situations. And they practice the age-old art of anatomical dissection to learn the basics of how their donors lived and died. Faculty, residents, fellows, and medical students can hone skills or learn new ones. Teachers can develop curricula that provide the best learning opportunities for their students then assess what’s been learned or what needs to be improved. “Simulation is transforming how we become doctors,” says Dr. Advincula.
- Log in to post comments